Understanding Bariatric Surgery: Making People Healthy Rather Than Thin
Professor Carel Le Roux has travelled in 2016 to Moscow to give a lecture on the mechanisms of bariatric surgeries, and to Australia, for a series of lectures discussing the topic of his newly published research paper in the British Medical Journal (BMJ) on why the NHS (National Health Service) in the UK should be doing more bariatric surgeries.
Le Roux is Professor of Experimental Pathology at UCD School of Medicine and UCD Diabetes Complications Research Centre at the UCD Conway Institute of Biomolecular and Biomedical Research . He has received the President of Ireland Young Researcher Award from Science Foundation Ireland as well as a Clinician Scientist Award from the National Institute Health Research in the UK .
The BMJ paper, which he co-authored is titled ‘Why the NHS should do more bariatric surgery; how much should we do?’
Bariatric surgery is an operation on the stomach and the bowel allowing the gut to send signals to the brain to make people feel full quicker after they’ve eaten. It is often viewed as a surgery designed merely to make people lose weight and become thinner. The bottom line of the paper is that these surgeries are about making people healthy rather than thin.
“It turns out that some people are very heavy but there is nothing wrong with them medically and to operate on them is not helpful because you can’t become healthier than healthy – but they may have all the potential side effects of the surgery,” explains Le Roux.
However, if operations are carried out on patients with complications of type 2 diabetes, especially those where medications weren’t good enough to prevent them from deteriorating, then surgery in conjunction with medication can lead to a much better outcome.
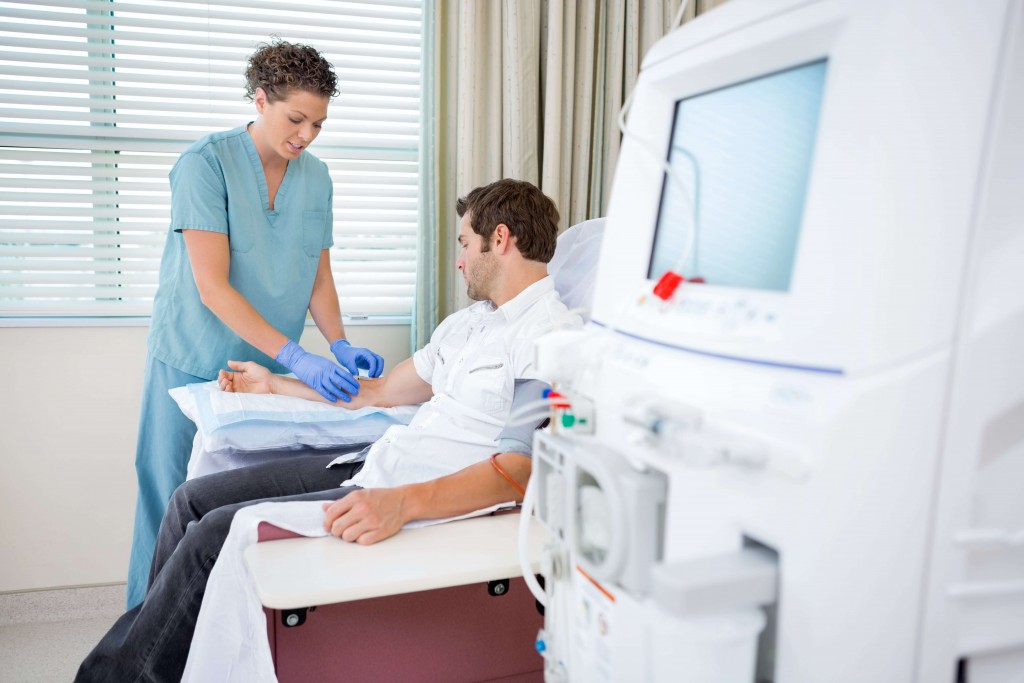
“To put this in perspective only 6% of the population in Ireland have diabetes but 10% of our healthcare expenditure is focused on diabetes. It’s not the recently diagnosed patients that cost money; it is the patients with diabetes with complications such as those needing renal dialysis.
“Dialysis for one individual costs almost €60,000 per year. If we carry out a €10,000 operation and we stop someone from going onto dialysis, we are effectively saving this expense and improving the person’s quality of life,” says Professor Le Roux.
Le Roux says that the healthcare expenditure of the HSE is in many regards similar to the NHS: bariatric surgery clinical services in the UK are similar to that in Ireland: “We have already invested in the infrastructure; there are two very good clinics at St Vincent’s University Hospital in Dublin and Galway University Hospital that have entire multidisciplinary teams ready and working so we don’t need additional investment in that. What we now need to do is to allow the patients to go through the existing systems to benefit.”
The BMJ paper points to the low level of bariatric surgeries being carried out by the NHS and argues the case for increasing this number, both for the patient’s benefit and the economic benefit. Right now the NHS is only doing about 8,000 operations per year. Our calculations suggest that they need about 50,000 operations per year to come in line with the number per capita being carried out in Sweden and France, where they have more mature healthcare systems.
“Right now the NHS is only doing about 8,000 operations per year. Our calculations suggest that they need about 50,000 operations per year to come in line with the number per capita being carried out in Sweden and France, where they have more mature healthcare systems.”
If we translate this to Ireland this would equate to about 4,000 operations per year but right now there are only 50 or so bariatric surgeries being carried out here. “Nobody is suggesting we jump from 50 to 4,000 right away; this is about starting a discussion on where we can have most impact both in terms of improving health and from an economic point of view.”
This discussion needs to be started, not least due to the misperception of obesity as a lifestyle choice rather than a disease. He says that obese patients are still being discriminated against significantly: “People will say ‘why should we spend money on operations when you can just tell them to eat less or do more exercise’. This is why interdisciplinary research is so important.”
Professor Le Roux and his research group at UCD receive significant funding from Science Foundation Ireland and the Health Research Board to investigate bariatric surgery and the mechanisms involved and they are also working with the UCD School of Philosophy and the UCD School of Agriculture and Food Science in order to have this interdisciplinary, societal impact.
“We have a responsibility to use tax payers’ money to do research that will impact positively on society and this BMJ paper is an example of such.”
Le Roux finishes: “I want to emphasise that this is not about making people thin or happy; it is to make people healthier and more functional and we, as doctors, often have to make difficult decisions. We have to say to patients that it’s not ‘first come, first served’, it’s about who needs it most.
We have a responsibility to use tax payers’ money to do research that will impact positively on society and this BMJ paper is an example of such.
“This has been defined in the paper by the diseases that get better after surgery. If you operate on someone with poorly controlled diabetes or blood pressure, or someone who is infertile due to their weight or has sleep apnoea, those diseases respond very well to surgery. Not everybody should have this kind of surgery. We need to operate on those who have diseases that will benefit most.”
This story first appeared in the summer 2016 edition of UCD Today, the university magazine.

